Cerebral Cavernous Malformation

Dr. Edward Smith and patient (photo courtesy of Boston Children’s Hospital)
Cerebral Cavernous Malformation (CCM) is one form of cerebrovascular disease. When you hear the terms cavernoma, cavernous angioma, cavernous hemangioma, or cavernous malformation, they are one in the same. CCM is also a benign vascular brain tumor. It is estimated that 1 in 100 people, or 3.5 million Americans, are affected by CCM, most of whom have no known genetic abnormality.
According to Dr. Mark Kahn, professor of cardiovascular medicine at UPenn, most patients learn they have the condition when they have a brain MRI for something unrelated, like a blow to the head. Some experience a symptom, like a seizure, because the CCM is leaking blood, or a stroke because it bursts. An aneurysm is similar, but it forms in an artery. Up to 20% of patients have a family history, and in them, the disease is much more aggressive. They may have a few of these malformations—or thousands. CCM is a major cause of stroke among younger patients, and even babies can have strokes when the blood-filled lesions burst.
Effective medical treatment that may limit disease progression is dearly needed, as available curative therapy is limited to surgical lesion eradication or stereotactic radiosurgery. Open skull surgery is currently applied to selected symptomatic lesions only (after hemorrhage or symptomatic lesion growth), but it is highly invasive with at times significant complications and unproven long-term benefit. Despite many research efforts, an effective medical therapy for this disease is still missing.
— Matteo Malinverno, senior post doc, IFOM, Milan, Italy
Questions and Answers:
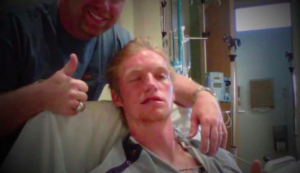
Ryan Westmoreland after his 1st craniotomy to remove a CCM
Is there any treatment for a CCM?
The primary treatment option for a CCM is surgical removal. Radiation therapy has not been shown to be effective. The decision to operate is made based upon the risk of approaching the lesion. For example, symptomatic lesions close to the brain surface in “non-eloquent” areas—not involved with motor function, speech, vision, hearing, memory, and learning—are very likely to be candidates for removal.
On the other hand, lesions located in deep brain areas are associated with higher surgical risk and are often not candidates for surgery until the lesion has bled multiple times. Medications can often lessen general symptoms such as headaches, back pain, and seizures.
What is the prognosis for patients with CCMs?

Ryan after his 2nd craniotomy to remove a CCM and his decision to retire from the Boston Red Sox.
Re-bleeding from a cavernous angioma is common, it is not predictable, and individuals frequently have multiple CCMs found via magnetic resonance imaging. Individuals with CCM are faced with a diagnosis that imparts risk of multiple future hemorrhages that occur seemingly at random and without any preventative therapy except surgical removal.
Why are brainstem tumors or lesions so difficult to treat?
The brainstem is a highly specialized and delicate area of the brain. The brainstem controls all our vital bodily functions. This includes breathing, heartbeat and swallowing. Depending on exactly where in the brain stem a tumor or lesion is located (and how big it is), surgery may not be possible without destroying a vital area of the brain stem, which would cause death.
Surgery for these tumors has developed a lot in recent years and is sometimes more successful than in the past. For some types of childhood brain tumors, a lot of progress has been made in treating them. But, when tumors are in the brain stem, it is still not usually possible to cure them.
Can benign brain tumors and lesions be life-threatening?
Benign brain tumors and lesions can be life-threatening. They can compress brain tissue and other structures inside the skull, and they may recur. The term “benign” can be misleading. Terminology is further complicated by some investigators who classify low-grade cancerous tumors as either “benign” or “relatively benign.” Regardless, compression of brain tissue or its additional structures (for example, nerves, ventricles) by a tumor mass is a major cause of the symptoms seen with benign, as well as malignant, tumors.
What are the symptoms of a benign brain tumor or cerebrovascular disease?
The symptoms of a brain tumor vary widely and depend on the specific type of brain tumor, location, rate of growth and size. There are no specific symptoms that only occur due to a brain tumor, but signs and symptoms may include:
- New onset or change in the pattern of headaches
- Headaches that gradually become more frequent and more severe
- New onset of seizures
- Gradual loss of sensation or movement in an arm or a leg
- Difficulty with balance
- Speech difficulties
- Personality or behavior changes
- Unexplained nausea or vomiting
- Blurred vision, double vision, or loss of peripheral vision
- Hearing problems
What are the causes?
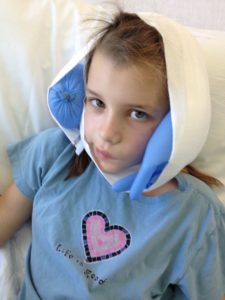
Riley Callen, our founder, after her 6th surgery to improve the facial palsy caused by her 2nd craniotomy to remove her brainstem-based CCM.
In most cases, we still do not understand what causes the genetic mutations that can lead to primary brain tumors. The following are some explanations of the risk factors that can increase the chance of developing a brain tumor:
- Age — Your risk of developing a brain tumor increases as you age. Brain tumors are most common in older adults. However, a brain tumor can occur at any age. Certain types of brain tumors, such as medulloblastomas and juvenile pilocytic astrocytomas, occur almost exclusively in children.
- Family history of brain tumors — A small portion of brain tumors occur in people with a family history of brain tumors or a family history of genetic syndromes that increase the risk of brain tumors.
- Exposure to radiation — People who have been exposed to a type of radiation called ionizing radiation have an increased risk of brain tumors.
- Immunosuppression — If your immune system is severely depressed due to disease, such as HIV. Powerful medications designed to shut down your immune system, such as those taken after an organ transplant, can also increase your chances of developing a brain tumor or other cancers.
Who is more likely to get a brain tumor, an adult or a child?
Brain Tumors do not discriminate. Primary brain tumors–those that begin in the brain and tend to stay in the brain–occur in people of all ages, but they are statistically more frequent in children and older adults. Brain tumors in children are different from those in adults, and consequently, are treated differently. As many as 69% of children will survive, but they are often left with long-term side effects.
